Feb 27
What Centenarians Reveal About Pain, Aging, and Meaningful Living
Empty space, drag to resize
Good day, friends.
After a recent conversation with a colleague, I’ve been thinking about pain—how we inherit stories about it, how those stories shape the way we age, and how the data keeps ambushing our assumptions.
That conversation led me back to a study I hadn’t looked at in a while. This one focused on 73 centenarians—average age 100.4—who were still able to self-report. The researchers measured functional capacity, cognition, mood, arthritis, and pain. Then they ran a hierarchical cluster analysis and found something surprising.
Let’s dig into it.

What did authors do?
1. Sample = 73 centenarians (mean 100.4 yrs) who could self-report.
2. Measured:
- Functional capacity – summed PADL + IADL (0–28)
- Cognitive capacity – short MMSE (0–21)
- Depressive symptoms – GDS-10 (0–10)
- Documented arthritis & 0-10 pain scale.
3. Hierarchical clustering → three phenotypes.
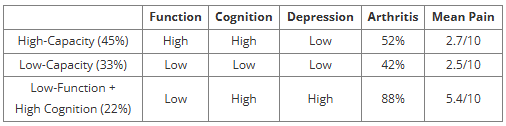
🔑 Two Key Takeaways
1. Pain—not aging—is the main disruptor.
After controlling for arthritis and pain, the tidy link between mood, function, and cognition disappeared. That’s important: it suggests that pain—not the aging process itself—is what’s driving distress in later life. The idea that “older = worse” didn’t hold up.
2. Cognitive sharpness can amplify suffering.
The most distressed group had the highest cognitive scores. These centenarians weren’t confused—they were clear-eyed about what they had lost. That very clarity may have made their experience of pain and decline more emotionally difficult.
⚠️ Limitations
It’s a small, German-only, cross-sectional study—so no sweeping claims here. But it’s a compelling reminder that we often conflate aging with inevitable decline, when it may be unaddressed pain doing the damage.

🧠 Rethinking Pain, Aging, and the Power of Social Connection
It’s easy—and common—for people to assume:
“As I get older, I’ll hurt more, move less, and feel worse.”
But this study tells a more hopeful, more nuanced story. So...
- Reframe “I’m just getting old” — pain is treatable, and aging doesn’t have to mean decline.
- High-functioning older adults may suffer more emotionally. Be ready to listen, validate, and reframe.
- Treat the pain, yes — but also ask about loneliness, purpose, and connection. This one is often missed.
We don’t stop moving because we grow old — we grow old because we stop moving, connecting, and finding meaning.
Empty space, drag to resize
🧬 Social Health - Three Key Studies Worth Considering
Yes, pain matters as we age—but how we cope with pain, and how much it interferes with life, often comes down to something deeper. That’s where resilience, connection, and social health step in. These elements don’t erase pain, but they can buffer its impact—helping people adapt, stay engaged, and protect their quality of life in the face of life’s inevitable challenges.
Let's review a few studies here:
Let's review a few studies here:
📌 Li et al. (2024) – Using data from the Chinese Longitudinal Healthy Longevity Survey, they found that socially isolated older adults were significantly less likely to reach age 100. Social connectedness — via family, friends, and community — was a stronger predictor of longevity than many traditional physical health metrics.
📌 Waldinger et al. – Harvard Study of Adult Development – Following people for over 80 years, this study found that strong, supportive relationships in midlife predicted better physical health, mental health, and longevity later in life. Social connection was more predictive of long-term health than cholesterol levels.
📌 Wang et al. (2024) – In a 10-year follow-up of over 15,000 older adults, those who increased their social participation (e.g., group activities, community involvement) had a 30% reduction in all-cause mortality. Again: connection is medicine.
Empty space, drag to resize
✅ What This Means in Practice
- Treat the pain – Use the evidence-based tools we already have. Don’t under-dose older adults—they can handle more than we think.
- Offer new perspectives – Help patients reframe aging as adaptation, not inevitable decline. Show them what’s still possible.
- Prescribe social health – Encourage connection, purpose, and community. Especially as people age, disconnection becomes a major risk factor.
🧩 When people are in less pain, they move more, engage more, and show up more.
🫶 And when they’re socially connected, they cope better—with pain, with loss, and with change.
Empty space, drag to resize
📌 Pain. Story. Support. Social connection.
Let’s lead with all four as we help people age with clarity, dignity, and less fear.

👨🏫 Case Study: "Frank", Age 80 – From “It’s All Downhill” to Coffee and a Comeback
Frank, a retired high school principal, came in with persistent low back pain. He believed his pain was just part of aging — that things would inevitably get worse — so he’d started letting go of the things he loved: golf, gardening, even weekly coffee with friends. I am sure many of you seen this pattern before!
“What’s the point,” he’d say. “I’m just getting older.”
But pain wasn’t the villain here — the story he believed about aging was.
We gently talked through that narrative. Using research from centenarian studies to draw on, we explored how pain is modifiable and that social health isn’t a luxury — it’s part of the prescription.
What shifted:
Frank started meeting his buddies again at the Italian café on the corner (as you do for a delicious coffee in East Vancouver). After a few weeks, the pain was still there — but he wasn’t as consumed by it. He had more laughs, more movement, and less mental load.
Eventually, a friend roped him into a round of golf. It hurt. But not enough to stop him from going again the next week. And the week after that, it hurt less.
Empty space, drag to resize
📌 The Principle:
Assumptions about aging shape behaviour — and behaviour shapes pain.
Frank thought decline was inevitable, so he stopped moving and connecting. Reversing that mindset — and re-engaging socially — didn't just help his mood. It helped his him heal.
Treat the pain. Explore the story. Prescribe connection.

🎧 Podcast: The Long Game – Sam Harris & Robert Waldinger
In this episode of the Making Sense podcast, Sam Harris converses with Dr. Robert Waldinger, director of the Harvard Study of Adult Development. They dive into the intricacies of well-being, discussing topics such as the limitations of self-reported data, the distinction between the experiencing and remembering selves, and the profound impact of relationships on physical health. Waldinger emphasizes that strong social connections are more predictive of long-term health than factors like wealth or cholesterol levels.
Empty space, drag to resize
For a comprehensive exploration, consider reading The Good Life, co-authored by Waldinger and Schulz. The book distills decades of research from the Harvard Study of Adult Development, highlighting how close relationships are central to happiness and longevity. It offers practical insights into nurturing these connections throughout life.

“Relationships aren’t just nice to have — they’re essential to health.”
In The Good Life, Waldinger and Schulz unpack decades of research from the Harvard Study of Adult Development. The standout insight? Strong relationships are the single best predictor of health and happiness across the lifespan.
One finding still echoes: chronic loneliness can be as harmful to your health as smoking 15 cigarettes a day.
But here’s the hopeful flip side — connection is medicine.
Whether it’s a weekly coffee with friends, a quick call to a sibling, or showing up to your walking group — these little moments build health just as surely as nutrition, movement, or medication.
It’s a gentle but powerful reminder:
If we want to help people heal, we need to think beyond pain and toward people.
Empty space, drag to resize
So here’s my final takeaway:
Treat the pain, shift the story, strengthen the ties. Because age isn’t the problem— avoidance and isolation are. It’s connection that keeps us grounded, resilient, and moving forward.
The real superpower?
A strong social buffer to ride out life’s tougher chapters.
Call a friend. Walk to coffee. Say yes to the invite.
The rest — movement, meaning, even a little less pain — tends to follow.
Until next time: Keep the coffee strong, the science honest, and your people close.
Stay nerdy,
Sean Overin, PT
Subscribe to our newsletter
Every Friday we cover must read studies, how they fit in practice, give it real world context, provide top resources and one sticky idea.
Thank you!
You have successfully joined our Friday 5 Newsletter subscriber list.
